What is Hirschsprung’s disease?
Hirschsprung’s disease is a developmental disorder of the nerves of the intestine. The intestine contains nerves in its wall. The nerves transmit signals to the muscle of the intestinal wall that allow the intestine to move its contents forward for digestion and removal (stooling). The specific nerves of intestinal movement are called “ganglion cells". In Hirschsprung’s disease treatment, there are no ganglion cells in the wall of the affected part of the intestine. Hirschsprung’s disease in Ahmedabad, Gujarat, Rajasthan.

Plain Xray abdomen showing dilated colon with sudden cutoff suggesting colon obstruction.
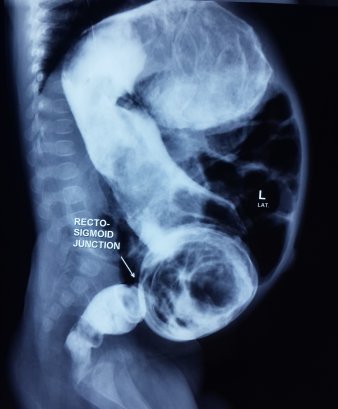
Contrast enema showing narrow aganglionic rectum and dilated normal colon.
If the nerves or ganglion cells are not present in a part of the intestine, that intestine does not move things through. The affected area acts like a blockage.
Variable length of intestine can be affected by this disease. The most common is Recto-sigmoid disease (80% of the total cases) in which the terminal few centimeters of large intestine is affected by the disease. The uncommon forms are long segment disease and total colonic aganglionosis (TCA).
What are the symptoms of Hirschsprung’s disease?
Early presentation;
- A newborn child normally passes stools within first 24 hours of birth. Delayed passage of meconium (black poo) is an important sign of Hirschsprung’s disease.
- Child may present in neonatal life or during early infancy with abdominal distension, constipation, poor feeding, or vomiting when feeding is attempted. Child may present with recurrent abdominal distension, foul smelling diarrhea and fever (enterocolitis) and rarely with intestinal perforation.
Late presentation;
- Some children with Hirschsprung’s disease present later in childhood with long standing constipation. This is most common in breastfed infants that typically develop constipation around the time of weaning. Clinical features in older children include poor weight gain, abdominal distension and dependence on enemas or suppositories to pass stool. Children with undiagnosed Hirschsprung’s associated constipation generally do not soil their underwear.
How common is Hirschsprung’s disease?
Hirschsprung’s disease is found in approximately 1 in 5000 children. Boys are commonly affected than girls.
What are the tests to be done?
The diagnosis of Hirschsprung’s disease is based on the clinical history, X-ray studies and a rectal biopsy.
Plain radiographs may suggest a distal bowel blockage.
Water-soluble contrast enema: In this study, a tube is gently placed in the rectum. Liquid dye (contrast) is injected to see if there is a narrowing of intestine (area where the nerves are not present) along with a distended intestine above the abnormal segment. This region is called where there is a difference in caliber of intestine (narrow abnormal segment and dilated normal segment) is called the “transition” zone—the transition between the narrow distal bowel with no ganglion cells and the proximal dilated colon. The study indicates approximately the length of colon without ganglion cells.
Rectal Biopsy: Full Rectal biopsy is the gold standard for the diagnosis of Hirschsprung’s disease. It is a minor surgical procedure performed under anesthesia. A small piece of rectum (terminal large intestine) is taken through the anus and the defect is closed with sutures. The biopsy is sent for examination by an expert histopathologist.
Manometry: In this study, the relaxation of the sphincter muscle will be measured. Lack of relaxation is suggestive of Hirschsprung’s disease.
What is the treatment of Hirschsprung’s disease?
The treatment of Hirschsprung’s disease is surgery, Hirschsprung’s disease in Rajasthan. The surgery involves removal of aganglionic (without nerves) intestine and connecting normal intestine with anus. The timing and type of surgical approach depend on expertise of the surgeon and condition of the baby.
A single stage trans-anal pull-through procedure is the current procedure of choice. The abnormal rectum and part of large intestine is removed through the anus and normal large intestine is joined with anus. A biopsy is sent from the normal looking intestine during the operation (intra operative frozen section) to confirm presence of ganglion cells in the part of intestine which is to be joined with anus. The whole procedure is completed without opening the abdomen in most of the cases.
The three stage procedure is employed when the baby is very sick, and has massive abdominal distension which is not relieved with rectal washouts. It is also employed when frozen section facility is not available.
What are the risks of surgery?
Bleeding, infection, anastomotic leak and intestinal obstruction are few of the risks which affect a few babies after the surgery.
What is the long term outcome?
The long term outcome is excellent. The problems like frequent stooling and constipation are encountered during first few years of life and usually settle after toilet training.
Anastomotic stenosis may require dilatation.
Enterocolitis may require hospitalization, antibiotics and IV fluids.

